We are thrilled to announce that Dr. Jessica Awerman has joined our team at Massachusetts…
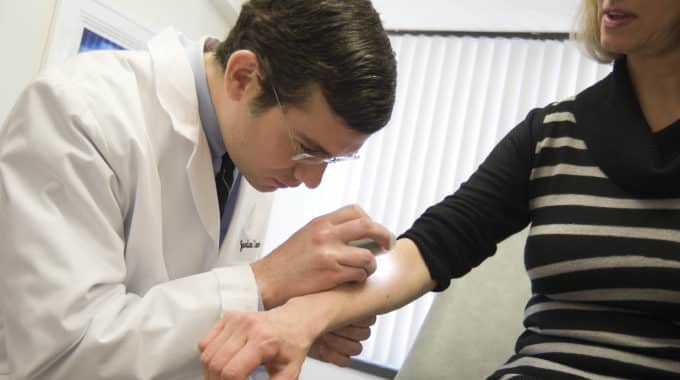
The Dermatoscope: Your Dermatologist’s Small Hand-Held Light
If you have been seen by a dermatologist for a mole check at Massachusetts Dermatology Associates, odds are you have probably seen your dermatologist reach into a white coat pocket and pull out a device that looks like a fancy flashlight. You might be wondering what your doctor is doing with this special light and the answer is that he or she is using it to perform “epiluminescence microscopy” (ELM) exam also known as dermoscopy (or dermatoscopy). The device not only magnifies and provides focused bright light, but also by polarizing the light allows us to better visualize the structures of the skin that are deeper than the outer surface.
As dermatologists, we rely on our eyes more than almost any other type of physician because the lesions we evaluate can be seen right on the surface of the skin. Most moles (nevi) and skin lesions can be easily assessed based on simple visual exam, but some require a closer look to decide whether the lesion is benign or atypical. In these cases the ability to see a slight depth into the skin can be of great aid in diagnosis. The ELM exam is of particular use in examining nevi with atypical features or lesions suspicious for melanoma. Features seen on ELM exam such as blue-white structures and atypical pigment patterns may alert us to lesions of concern, whereas more typical characteristic pigment patterns can reassure us that the lesion is benign.
Dermoscopy is an excellent tool that allows the dermatologist to see deeper than the skin surface, but just like standard visual exam it has limitations. In many cases the diagnosis may remain uncertain even after ELM exam. In these cases the patient may be offered the option of biopsy which allows the tissue to be viewed by a dermatopathologist who can take an even deeper look at the tissue under a microscope.
Using our eyes, our dermatoscope, and with the help our pathology colleagues, we are able to accurately classify and subsequently treat potentially harmful skin lesions.


