Skin Cancer Treatment
At Massachusetts Dermatology Associates, skin cancer treatment for our North Shore patients is a top priority. We understand that getting a diagnosis of skin cancer can be a frightening experience, and we pride ourselves in helping our patients step by step through the skin cancer treatment process:
- Clinical Diagnosis
- Skin Biopsy Procedure
- Analysis of Pathology Reports
- Communication of Results
- Treatment Options
- Skin Cancer Prevention
Our board-certified dermatologists have performed tens of thousands of skin exams and are experts in the diagnosis of skin cancer
Skin biopsies are performed with minimal patient discomfort. Biopsy specimens are sent to world class laboratories for pathology analysis by fellowship-trained dermatopathologists who generate a report that is sent back to our dermatologists.
Our dermatologists analyze the pathology reports and generate treatment plans specific for the patient. We have extensive experience with all types of skin cancer and special expertise with basal cell carcinoma, squamous cell carcinoma, and melanoma.
A phone call from our staff to each and every patient who has undergone a biopsy is made communicating, in detail, the results of the biopsy and the skin cancer treatment plan.
A wide array of skin cancer treatment options are offered depending on the type of skin cancer, the location of the skin cancer, and other factors specific to each patient. We offer Mohs surgery, surgical excisions, electrodessication and curettage (ED&C), along with other skin cancer treatments when medically appropriate.
Preventative therapies are often advised such as photodynamic therapy (BLU-U PDT) to attempt to prevent future skin cancers.
Do you have a question for one of our board-certified physicians at Massachusetts Dermatology Associates? Why travel into Boston, when you can have Boston’s best in Beverly MA? Call (978) 225-3376 to schedule an appointment.
Helpful Links
Mohs Surgery: Find out what to expect if you undergo this procedure for basal cell treatment or squamous cell treatment, especially in cosmetically sensitive areas such as the face, scalp, neck, hands, and feet.
Excisional Surgery: Find out what to expect if you undergo this procedure for basal cell treatment or squamous cell treatment.
Photodynamic Therapy (BLU-U PDT): Learn more about this popular and effective way to treat pre-cancerous lesions on the face, scalp, and arms.
Basal Cell Carcinoma (BCC)
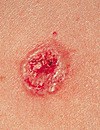
BCC is the most common type of skin cancer, with approximately 2,000,000 cases in the United States every year. Fortunately, this type of skin cancer generally grows very slowly and rarely spreads to other organ systems. Basal cell carcinoma can have a variety of appearances ranging from translucent papules with prominent blood vessels to chronic skin erosions.
Squamous Cell Carcinoma (SCC)
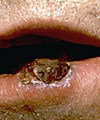
SCC is the second most common variety of skin cancer with approximately 500,000 cases in the U.S. per year. Like BCC, squamous cell carcinoma typically has a favorable outcome; however, approximately 2% of SCCs can spread to other organ systems. Squamous cell carcinoma, like basal cell carcinoma, can have a variety of appearances ranging from scaly patches (resembling eczema) to warty-appearing papules
Treatments of BCC and SCC
Like many other skin cancers, BCC and SCC are caused (in most cases) by sun exposure, and aggressive sun protection can go a long way to preventing these cancers. After skin biopsy, which is required to confirm the diagnosis, these skin cancers can be treated in several ways. Basal cell treatment and squamous cell treatment is often accomplished with Mohs surgery if they are on the head, neck, hands, or feet or if they show concerning microscopic features on the biopsy. Alternatively, basal cell treatment and squamous cell treatment can also be accomplished with surgical excision when they are located elsewhere on the body. Treatment with Mohs surgery or surgical excision often (but not always) entails the use of sutures (stitches) to close up the wound after surgery which will require patients to abstain from vigorous exercise or stretching of affected areas for one to two weeks after surgery when the sutures are removed. For patients who would prefer to avoid activity restrictions, some basal cell treatment and a subset of squamous cell treatment can be accomplished with electrodessication and curettage (ED&C) which entails scraping and burning of the skin cancer in three successive cycles and is nearly as effective as surgical excision but may results in less favorable scarring (but no sutures necessary). Treatment with the above techniques is highly effective with cure rates ranging from 93%-95% with ED&C or surgical excision to 98-99% with Mohs surgery. After the diagnosis of BCC or SCC, patients are advised to return for semi-annual full skin exams to monitor for cancer recurrence and the potential development of new skin cancers.
Melanoma
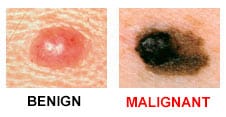
Melanoma is less common than BCC or SCC, with approximately 100,000 cases per year in the United States. Unfortunately, unlike SCC and BCC, melanoma, when not detected early enough is more likely to spread to other organ systems which has the potential to lead to severe disability or death. Melanoma, like SCC and BCC, can have a variety of appearances, and therefore those with a personal or family history of melanoma, and those with other risk factors for melanoma (e.g. history of blistering sunburns, extensive sun exposure, history of radiation therapy, history of immunosuppression, etc.) are encouraged to undergo regular skin surveillance with a dermatologist
Treatment of Melanoma
After a melanoma is diagnosed, the first step is careful interpretation of the pathology report to assess risk of melanoma spread to other organs (metastasis). Several factors are taken into account to determine the risk of a melanoma spreading beyond the site of the initial cancer. For low risk lesions, a surgical excision is performed at Massachusetts Dermatology Associates with adequate margins to maximize the possibility of cure. With regular skin surveillance, we tend to catch melanoma in the early stages, and cure rates for many of these lesions are upwards of 90%. For higher risk lesions, we often collaborate with our colleagues in surgical oncology to perform an additional procedure called a sentinel node biopsy which is used to further risk stratify patients and determine if, in addition to excision of the primary melanoma, whether other treatments are necessary.